Physiology of Kidneys
Kidneys from urine by filtration and secretion of waste materials from the blood. In addition, the selective reabsorption by tubular cells contributes to the maintenance of homeostasis (regulatory activities of kidneys).
1. Formation of Urine
The nephrons of the kidney perform this function. Primarily, three processes are involved in the formation of urine, glomerular filtration, tubular reabsorption and tubular secretion.
(a) Glomerular filtration: This occurs in the glomerular capsule. The barrier between internal portion of Bowman’s capsule and the blood present in the glomerular (the blood capillaries) act as an ultra filter. This barrier is composed of endothelial cells of capillaries, its basement membrane and the podocytes that form the inner portion of Bowman’s capsule. The ultra filter is highly permeable and allows free passage of water and solutes in blood plasma into the capsular space; forming the glomerular filtrate. The pore size of ultra filter is the only limitation for passage of solutes in blood plasma into the filtrate. Thus, the blood cells and plasma proteins are not filtered; hence except these constituents the composition of filtrate is same as that of plasma.
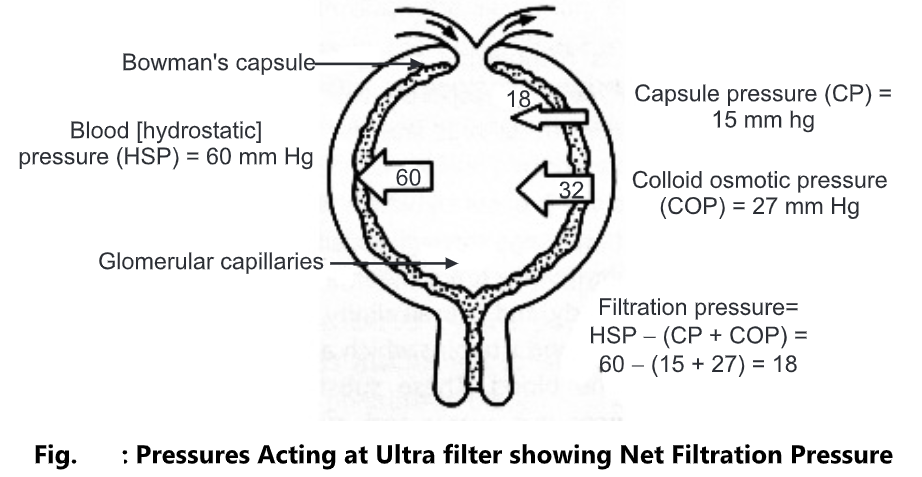
Three different pressures are acting at this ultra filter. These are of different magnitude and the sum total of these is the net filtration pressure. The major with highest magnitude of these is the capillary blood pressure (hydrostatic pressure). It is about 60 mm Hg. The diameter of efferent arteriole is smaller than that of the afferent arteriole and this generates the hydrostatic pressure under the influence of which the filtration occurs.
Two other pressures oppose this hydrostatic pressure; the oncotic pressure of blood plasma in capillaries; and the glomerular filtrate pressure. The plasma proteins are not filtered and they exert an oncotic (osmotic) force that opposes the filtration. This force is of about 27 mm Hg. The glomerular filtration formed exerts pressure on the ultra filter in opposite direction and is about 15 mm Hg. The resultant net filtration pressure is thus, 60 – (27 + 15)= 18mm Hg.
The amount of filtrate produced is about 120 ml/min. Thus, about 170-180 litres of filtrate is formed in 24 hours in case of normal adults. The urine output is 01 ml/min, i.e. about 01.5 litres in 24 hours; indicates that out of about 180 litres of filtrate; about 179 litres is reabsorbed by renal tubules.
Glomerular Filtration Rate (GFR)
The amount of filtrate formed in both kidneys per minute is called GFR. It is 120 ml/min or 180 litres per day. GFR depends on Net Filtration Pressure (NFP) which in turn depends on capillary blood pressure (Hydrostatic pressure). The capillary hydrostatic pressure mainly depends on the difference in the diameter of afferent and efferent arterioles, and the systemic blood pressure. Although systemic blood pressure may vary, the pressure in the glomerular is maintained by alterations in the lumen (diameter) of the efferent arteriole as compared with the afferent arteriole. Thus, even in hypotension the filtration continues so also in hypertension filtration occurs at normal rate. This ability of kidneys to maintain a constant blood pressure and GFR irrespective of changes in systemic blood pressure is referred to as renal ‘autoregulation.’
The juxtaglomerular apparatus is responsible for renal autoregulation. The enzyme ‘rennin’ is secreted by juxtaglomerular cells in response to different stimuli; the unknown vasoconstrictor substance released from these cells and the hormone angiotensin II are all responsible for renal autoregulation function.
(b) Tubular reabsorption: It is the process by which the composition and volume of glomerular filtrate is altered during its passage through tubule. The purpose of this process is to re-absorb the constituents of filtrate which are essential to the body, to maintain the fluid and electrolyte balance of the body and the alkalinity of the blood. The substances such as glucose, amino acids, fatty acids and vitamins which are more useful to the body are completely re-absorbed back into the blood. These substances are described as high threshold substances. Some substances, e.g. water and mineral salts are reabsorbed in varying amounts according to the physiological need of the body. Waste products such as urea and uric acid are absorbed only to a slight extent. These are called low threshold substances. Some substances, e.g. creatinine sulphate are not at all reabsorbed.
The tubular cells are responsible for reabsorbing materials from filtrate back into the blood. Reabsorption occurs by both active and passive diffusion and even by osmosis. The active process involves carriers within tubular cells; and transports only a limited amount of material per unit time. If the substance to be transported is present in excess of the limits of transportation such excess substance will appear in the urine.
Tubular reabsorption varies in different parts of the tubule as shown in the table below.
| Tubular reabsorption | ||
| Part of tubule | Mechanism of reabsorption | Substance reabsorbed |
| 1. Proximal convoluted tubule. | a. Active transport | Glucose, amino acids, vitamins, bicarbonates, sodium. |
| b. Passive diffusion | Chloride, sulphate, phosphate and urea. | |
| c. Osmosis | Water (obligatory water reabsorption). | |
| 2. Loop of Henle | a. Active transport | Chlorides (Cl–) and Potassium (K+). |
| b. Passive diffusion | Sodium (Na+) – first -by Passive diffusion into the tubular cell and then by active transport to blood. | |
| 3. Distal convoluted tubule and collecting tubule. | a. Active transport
| Sodium (Na+ ) in exchange for K+ or H+ . |
| b. Hormonal influence | Facultative reabsorption of water. | |
(c) Active secretion: Tubular cells actively secrete certain substances into the filtrate. This secretion is aimed at getting rid of certain materials and controlling blood pH. The substances secreted by tubular cells include Potassium (K+), Hydrogen (H+) ammonium ions (NH4+) and creatinine.
2. Water Balance
Water constitutes about 60 percent of adult human body weight. It is distributed in the body in three main compartments, i.e.
| Blood plasma Interstitial fluid Intracellular fluid | 5% 11% 44% | The figures are in terms of adult male |
Water is taken into the body through the alimentary canal and a small quantity is also produced by the metabolic process in the body. Water is excreted from the body in the expired air, as a constituent of faeces, as sweat, through the skin and through urine. The amount of water excreted in expired air and in faeces is fairly constant. Water excreted in the sweat is associated with the maintenance of body temperature. The balance between intake and output is maintained by the kidneys. Normally, fluid output is directly related to fluid intake. Water loss through kidneys is rigorously controlled and varies from 1000-1500 ml in 24 hours. This output is mainly controlled by the antidiuretic hormone (ADH). This hormone is produced and released into the blood by the posterior lobe of the pituitary gland. The osmotic pressure of blood is always maintained constant. Any increase or decrease in the intake of water, affects the osmotic pressure of blood.
If the osmotic pressure of the blood is raised, the osmoreceptors in the hypothalamus are stimulated. There is a close link between hypothalamus and posterior lobe of pituitary gland. The stimulation of osmoreceptors in hypothalamus results in increased output of ADH by the pituitary gland. Conversely, if osmotic pressure of blood is reduced, the release of ADH in the blood is reduced. The ADH acts on the tubules of the kidneys which increase the permeability of distal and collecting tubules. This results into increase in reabsorption of water from tubule into the circulating blood. Increase in the concentration of dissolved substances in the blood increases the production of ADH, resulting in reabsorption of water which dilutes the blood. The effect of diluting the blood is to reduce the amount of ADH produced. The cyclic effect maintains concentration of ADH in the blood within narrow limits.
Although the antidiuretic hormone is an important means by which the water balance of the body is maintained, it is not the only one. If there is an excess amount of any dissolved substance in the blood, it is excreted through the kidneys and excess of water is excreted with it; for example, in case of untreated diabetes mellitus. Also, if excess amount of electrolytes have to be excreted from the body, the amount of water required for this purpose is increased. This may lead to dehydration, inspite of increased production of ADH, but it is usually accompanied by acute thirst and increased water intake.
3. Electrolyte Balance
Changes in the concentration of electrolytes in the body may be due to changes in the amount of water or the amount of electrolytes. Sodium is the most common of the cations that exists in the extracellular fluid. As it is excreted through urine, its balance in the body is maintained by kidneys. When the amount of sodium is decreased, aldosterone production is increased and an increased amount of sodium is reabsorbed by kidneys. The secretion of aldosterone is influenced by ACTH from pituitary gland by a fall in the concentration of sodium in the blood and the rennin produced in the kidneys.
4. Maintenance of the Blood Pressure
The Juxtaglomerular cells in the kidney are responsible for this function. When the blood pressure decreases, it causes the release of hormone rennin by the kidneys. Renin reacts with globulin in the blood and forms angiotensinogen which in turn forms angiotensin-l. It stimulates the adrenal cortex to produce the hormone aldosterone which causes increased reabsorption of sodium. This is followed by reabsorption of water; the blood volume increases, thereby increasing the blood pressure. The angiotensin-I is converted into angiotensin-II by the enzymes in the lungs. Angiotensin-II is a powerful vasoconstrictor and increases blood pressure. Thus, the blood pressure is maintained.
Components and Characteristics of Normal urine | ||
Components | Percent Composition | Amount in 24 hours urine sample |
| 1. Water | 95 | 950-1430 ml |
| 2. Urea | 02 | 20-35 g |
| 3. Creatinine | 0.075 | 01-01.5 g |
| 4. Uric acid | 0.05 | 0.5-0.8 g |
| 5. Sodium ions | 0.35 | 03.5-06 g |
| 6. Potassium ions | 0.15 | 02-03.5 g |
| 7. Calcium ions | 0.015 | 0.01-0.3 g |
| 8. Ammonium ions | 0.04 | 0.08-0.5 g |
| 9. Magnesium ions | 0.006 | 0.06-0.08 g |
| 10. Chloride ions | 0.6 | 06-09 g |
| 11. Phosphate ions | 0.15 | 01.5-02.5 g |
| 12. Sulphate ions | 0.18 | 01-015 g |
| 13. pH | – | 04.8-07.4 |
| 14. Specific gravity | – | 01.016-01.02 |
| 15. Volume | – | 1000-1500 ml |
Ureter
The ureter commence from hilum of the kidney as upper funnel shaped end known as renal pelvis. The collecting ducts of nephrons open into papillary ducts which in turn open into minor calyces. The minor calyces join to form major calyx; two or three such major calyces unite to form the renal pelvis. The renal pelvis extends downwards as a small tube of 04-05 mm in diameter. Each ureter is about 25-30 cm in length and opens into urinary bladder. The ureter pass obliquely through the wall of urinary bladder. When bladder is full of urine the pressure compresses the urethral openings and prevents the backflow of urine into ureter. Three coats of tissues that form the ureter are the outer fibrous coat, middle muscular coat and an inner mucous lining. The mucous lining is composed of transitional epithelium and mucous secreted by its cells act as protective coat over those cells, preventing their contact with urine. The peristaltic contractions of muscle coat propel the urine to the urinary bladder.
Urinary Bladder
It is a hollow muscular organ situated in the pelvic cavity posterior to the symphylids pubis, anterior to rectum in male and anterior to neck of uterus and vagina in female. Its shape depends on amount of urine it contains; when empty it collapses and when accumulation of urine occurs it goes on distending. When it is full of urine, it is ovoid in shape and rises considerably up in the abdominal cavity.
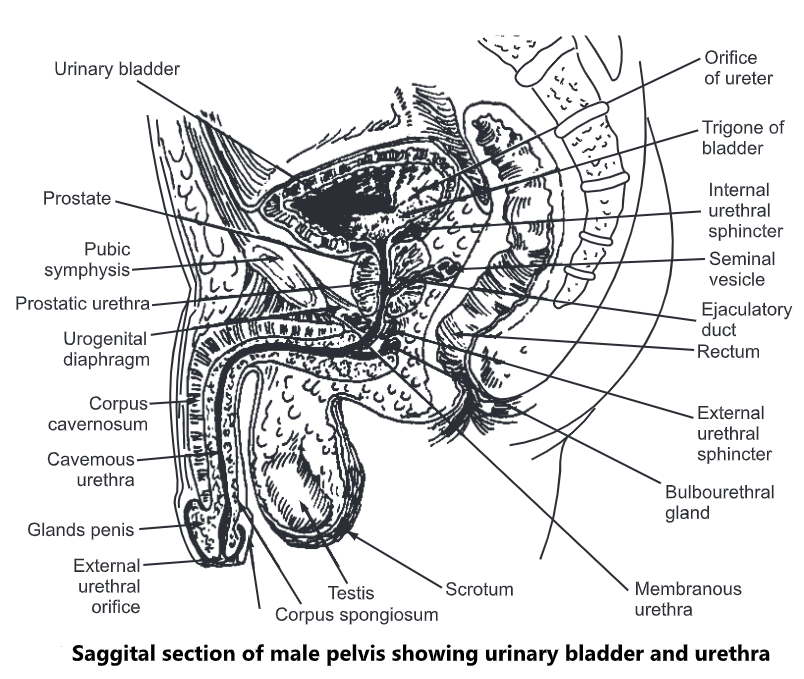
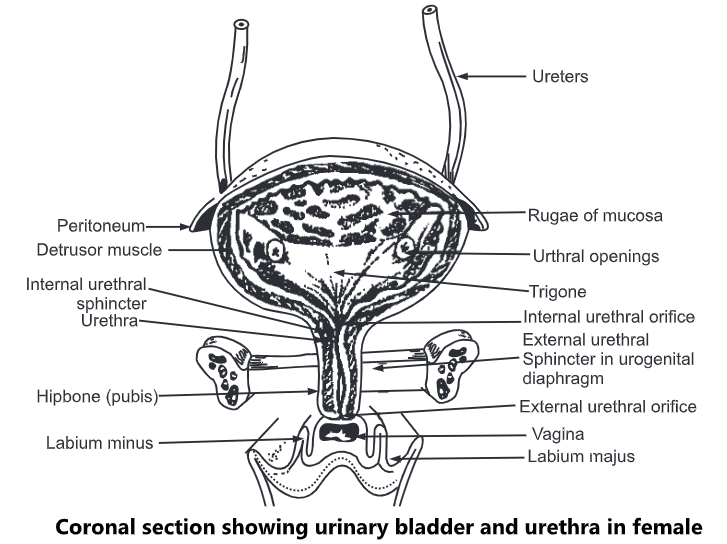
Urinary bladder has four coats:
(1) The innermost is the mucous lining formed of transitional epithelium, which shows folds (rugae) except in small triangular part formed between the openings of ureter and the orifice of urethra. This triangular part is known as trigone. The folds allow the distension of bladder as urine accumulates in it.
(2) The submucous coat is made up of connective tissue that connects inner mucous coat with the outer muscular coat.
(3) The muscle coat has three layers of smooth muscles: inner longitudinal, middle circular and outer longitudinal. At the urethral orifice the circular muscle forms an internal urethral sphincter.
(4) The outermost serous coat is a reflection of peritoneum and covers only superior surface and the upper parts of lateral surfaces of bladder.
The bladder is supplied by autonomic nerves from both the branches of autonomic nervous system (craniofacial and thoracolumbar). The reflex centres of these fibres are located in the midbrain, anterior pons and hypothalamus. The impulses froms these nerves are responsible for contraction of bladder and relaxation of internal urethral sphincter.
The bladder functions as a reservoir for urine.
Urethra
The urethra is a muscular tube that extends from inferior surface of urinary bladder and carries urine to the exterior of the body. At the pelvic floor when it passes through the muscle, (urogenital diaphragm) it is surrounded by the external urethral sphincter.
In females, it is a narrow membranous canal extending from bladder to external orifice the meatus, and about 03.8 cm in length.
It is placed obliquely downwards and forwards along the anterior wall of vagina. The meatus is the narrowest part and is located between the clitoris and the opening of the vagina.
The walls of the urethra have three coats:
(1) Outer muscular coat which is continuous with that of the bladder.
(2) Middle thin layer of spongy tissue and
(3) Inner mucous coat.
The male urethra is about 20 cm long and depending on location it is described as having three parts:
(1) Prostatic; which runs vertically through prostate gland,
(2) Membranous which extends between prostate to urogenital diaphragm.
(3) The cavernous portion, which extends from membranous to the urethral meatus.
Micturition
The act of passing the urine to the exterior is called as micturition. It is carried out by both voluntary and involuntary nerve impulses. When urine accumulates in the bladder, sufficiently (about 300 ml) it results into stretching of bladder wall and stimulates the nerves to initiate sensory impulses transmitted to the lower portion of the spinal cord. These impulses by way of sensory tracts to the cortex, initiate a conscious desire to expel urine. By way of micturition reflex, of which the centre is in sacral spinal cord; the bladder muscles are stimulated to contract and the internal urethral sphincter to relax. By way of sensory tracts to the cortex the conscious desire to expel urine is felt. These higher centres in the brain can voluntarily control contraction or relaxation of external urethral sphincter. When voluntarily external urethral sphincter is relaxed, the micturition occurs.
Pathophysiology of Renal Diseases
Glomerulonephritis is an inflammatory condition, possibly of allergic origin. Glomeruli are the main targets. Oedema may be present in both the acute and sub-acute stages of nephritis. This stage is called dry nephritis. The cause of oedema is as follows : Two, more or less equal but opposite, forces are always at work in the fine capillaries.
(a) Blood pressure, which tries to force the fluid part of the blood through the vessel wall into the tissues.
(b) The osmotic pressure of the blood proteins which holds the fluid back with the vessels.
In nephritis, the blood proteins are seriously diminished because of albuminuria. This reduces the osmotic pressure. As a result, more fluid is forced through the vessel wall into the tissues resulting in oedema. If the site of damage is tubules, rather than glomeruli, it is called tubular nephrosis. It involves combination of albuminuria and massive oedema. Pyelonephritis involves inflammation of the kidney and the renal pelvis. The inflammation is primarily of the interstitial tissue. The case is an infection by pyogenic bacteria, particularly E. coli, Streptococci and Staphylococci. It is one of the commonest forms of renal diseases. In chronic conditions, hypertension may develop. The hypertension caused by glomerulonephritis or pyelonephritis is called secondary hypertension.
A urinary calculus is a stone that is formed in the urinary tract. It may be formed either in the kidney or in the bladder. The symptoms include pain, the passage of pus and blood through urine and is an evidence of renal failure.
Oedema
All the cells in the body are bathed in the tissue fluid. It serves as a medium of exchange between blood plasma and the cells. The tissue fluid is derived from the plasma of the blood. As walls of blood capillaries are thin, some of the fluid passes out into the space between the tissue cells. This occurs by means of diffusion and by capillary hydrostatic pressure. Another force, called protein osmotic pressure is formed by the plasma protein which acts as a pulling force to hold the fluid in the vessel as well as to attract fluid in. This opposite force prevents undue loss of fluid from the capillaries. As blood moves through the capillary network and some fluid is lost in the tissue space, the plasma protein concentration is slightly increased and hence the pulling force is increased. As a result, the water and cystalloids re-entering in the capillaries colloids with water and enter the lymph capillaries. Thus, normally there is a delicate balance between the fluid leaving and re-entering the capillaries. The disturbance in this balance causing decrease in fluid return in the capillaries results into the excess accumulation of tissue fluid called oedema. The oedema may arise from the following reasons —
(1) Excessive mechanical hydrostatic pressure in the capillaries, if venous drainage is blocked;
(2) Decrease in osmotic pressure due to insufficient plasma proteins;
(3) Blockage of lymphatics;
(4) Damage to the capillary walls so that plasma proteins leak out into tissue spaces and
(5) An important factor causing oedema is the inability of kidneys to excrete sodium.
The basic treatment for oedema is the administration of diuretics, which are drugs that increase the quantity of urine production.
