Lactation
Lactation (milk production in mammals) comprises two phases: lactogenesis (the initiation of milk secretion) and galactopoiesis (the maintenance of established lactation).
▶Mammary glands
Ducts in the mammary glands develop after puberty, under the influence of estrogens, growth hormone and adrenal glucocorticoids. During pregnancy, the mammary glands enlarge and alveoli develop in response to increasing levels of estrogens, growth hormone, adrenal glucocorticoids, insulin, progesterone and (from the placenta) somatomammotropin.
▶Lactogenesis
Prolactin (from the anterior pituitary) stimulates lactogenesis; before birth placental secretions of estrogens and progesterone inhibit milk production. After the expulsion of the placenta from the womb, estrogen and progesterone levels fall and lactogenesis commences.
▶Galactopoiesis
Continued galactopoiesis requires growth hormone, parathyroid hormone and cortisol which facilitate provision of amino acids, fatty acids and calcium. In women, milk release does not begin until 24–72 hours after birth, the expulsion of the baby being the stimulation. During the first 24–72 hours the baby receives colostrum. Colostrum has high levels of proteins and is present in the mammary glands when the baby is born. Colostral components include laxatives which encourage the elimination of fetal wastes (e.g. mucus, bile and dead gut epithelium cells) from the gut. Hormones to facilitate development of the neonatal digestive system are contained in colostrum (and, later, milk). Human colostrum (and, later, milk) has high levels of IgA antibodies and confers passive immunity to the infant.
The maternal IgA remains in the gut where it neutralizes gut pathogens: IgA, greatly helped by other colostral components such as lactotransferrin, acts on harmful microorganisms such as coliform bacteria (e.g. Escherichia coli): breast-fed human babies have less than 20% of the mortality of bottle-fed babies from coliform pathogens. Immune cells (macrophages, neutrophils and lymphocytes) are also transferred in colostrum and milk. Such B lymphocytes include IgA-secreting cells, particularly responsive to gut pathogens (e.g. E. coli K1 strain which causes 84% of infant meningitis).
Other species may not transfer IgA; cow milk contains maternal IgG which can be transported across the calf gut wall to enter the calf’s circulation. Human milk comprises 88% water, 6.5–8% carbohydrate, 1–2% protein, 3–5% fat and 0.2% salts. Milk in marine mammals (e.g. seals and whales) is very rich in fats and enables the newborn animals to build up insulating blubber very quickly. Seal milk contains 57.9 g of fat per 100 g of milk, compared with 3.7 g of fat per 100 g of cow’s milk.
▶Suckling
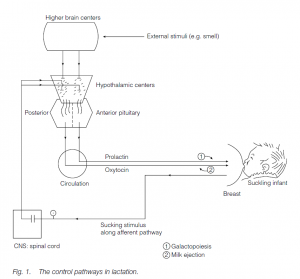
Nervous signals from the sucking action on the nipples or teats pass to the mother’s hypothalamus and cause a surge of prolactin from the anterior pituitary gland which lasts, in women, for about 60 minutes. This acts on the mammary glands to provide milk for the next suckling period. Stimulation of the hypothalamus by sucking also results in the secretion of oxytocin via the posterior pituitary.
Oxytocin causes the smooth muscles in the mammary glands to contract, expelling milk from the alveoli: stronger sucking results in stronger alveolar myoepithelial cell contraction and milk expulsion, an example of positive feedback. (Mammary glands which are not emptied soon stop galactopoiesis: in women, lactation can continue for over 2 years, although the rate of galactopoiesis slows after about 8 months.). Lactation helps the uterus to contract following birth by suppressing production of gonadotropins and sex steroids; menstruation may not occur in nursing mothers, although over 50% of women do ovulate while lactating.