Keeping in view the prevalant common situation whereby the recipient happens to reject the ‘donor graft’, the reverse may also take place when the said donor graft essentially comprises of immunocompetent cells. In immunological environment this specific phenomenon is invariably known as graft-Vs-host disease (or reaction). The net result is normally displayed and characterized by the ‘graft’ immunologically rejecting the ‘host’. Examples : The above very commonly occurring phenomemon may be explicitely explained with the help of the following typical example :
(1) A patient being administered with fresh bone marrow from a non-identical donor, evidently in such a situation the patients existing immune cells shall attack the ‘grafted cells’, whereas the grafted bone marrow cells will attack normal body tissues very much present within the patients body. Hence, in this specific instance it is absolutely necessory to first completely destroy the entire immune cells of the patient by subjecting him to whole-body X-Ray irradiation treatment just prior to his receiving the bone-marrow graft so as to protect the ‘graft’ from any external attack. Besides, it is equally important and vital that the patient’s tissues may also have to be adequately protected from attack by the prevailing immune cells in the bone marrow graft. If by any chance this protection to the patient’s tissues are not accomplished duly, there could be a serious lethal condition developed ultimately usually termed as graft-Vs-host disease (GVHD). In order to avoid, manage and control this condition from the very grass-root that pre-operative corrective measures should be swung into action to suppress the immune responsiveness of the grafted cells by the help of appropriate ‘drugs’. However it is quite necessary and important that the dosage regimen of the drug must be reduced slowly and gradually over a certain length of time till the ‘graft’ is rendered fully tolerant and totally acceptable in its new environment.
Ultimate prevention of GVHD essentially needs an extremely sensitive and careful balancing of the immunosuppressive drugs therapy for relatively longer span wherein the patient is required to be confined in an isolated sterile environment. It has been observed that the immunosupressive drugs do possess two serious drawbacks, namely : (a) rendering the patient quite vulnerable to infection ; and (b) exerting enormous unpleasant side-effects. However, the discovery of a new drug cyclosporin A has considerably eased the situation which is found to be both more effective and having relatively fewer side-effects.
(2) Leukemia and GVHD : Leukemia has been pronounced as one of the most dreadful diseases ; and the extension of longivity vis-a-vis a positive hope of complete cure particularly in adults may be accomplished successfully by replacing the patient’s abnormal bone marrow with healthier cells. It has been duly observed that only a small fraction of the patient’s bone marrow actually made up of malignant (i.e., cancerous) cells. Therefore, logically and ideally such a grave condition may be tackled by adopting the three vital steps in a sequential manner, namely : (a) removal of the bone marrow ; (b) destruction of the leukemia cells ; and (c) replenishing the healthy cells to the original subject. In fact, such a streamlined meticulous stepwise operation shall not only minimise drastically the higher chances of survival and the utmost danger of GVHD, but also to negate the requirement for inducing immunosuppression.
Though substantial break throughs have already been accomplished and reported, such as : cleaning up of bone marrow by employing monoclonal antibodies to neoplasm (tumour) determinants which are strategically attached to toxins, radioisotopes or magnetic beads, that could be detached and removed subsequently along with the cancerous cells to which they get intimately bound by means of the electromagnets. In nut shell, one has to travel a long zig-zag path to hit bull’s eye i.e., to lay its hands on to an absolutely fool-proof, doubly sure and efficient means of ‘immunotherapy’.
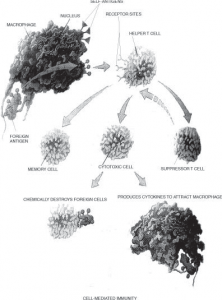
Figure above ↑ designates the summarized form of the ‘cell-mediated immunity’ whereby the regulatory and the cytotoxic activities of T cells during the specific immune response. This process requires approximately 36 hours to reach its full effect. Unlike B cells, T cells cannot recognize foreign antigens on their own. A foreign antigen is normally recognized by a macrophage that engulfs it and displays part of the antigen on its surface next to a histocompatibility or ‘‘self’’ antigen (i.e., macrophage processing). The very presence of these two markers together with the secretion of a cytokine, interleukin-1 (IL-1) by macrophages and other antigen-presenting cells (APCs) activaties specifically CD4+/CD8– T cells [helper T cells (TH)], that modulate the activities of other cells involved in the ensuing immune response significantly.
